A medical, science-based perspective on early skin aging and collagen degeneration.
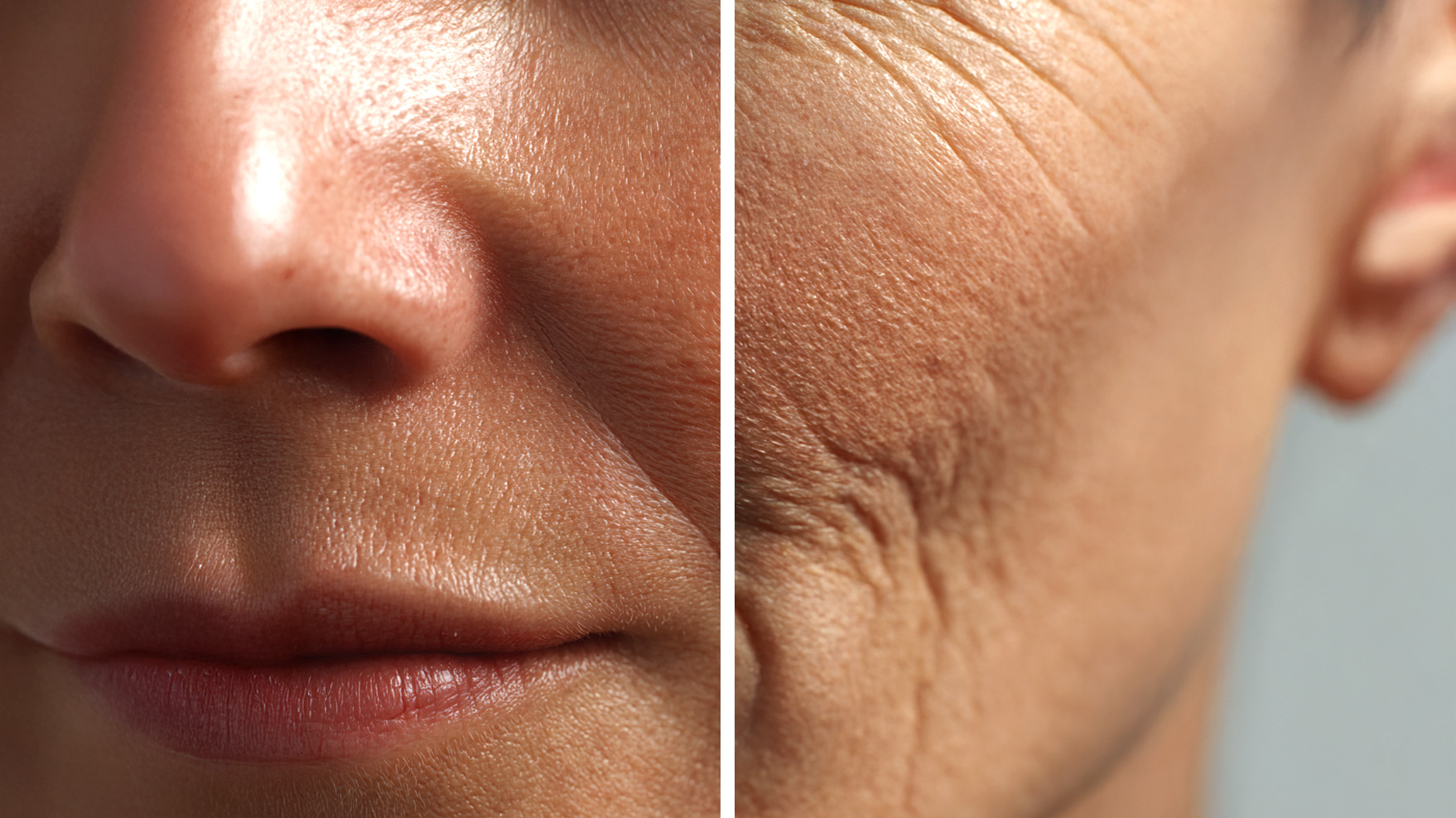
Many people begin to notice subtle changes in their skin in their early 30s: fine lines, reduced firmness, less elasticity and a gradual loss of glow. These changes are not random. They reflect a well-documented biological process:
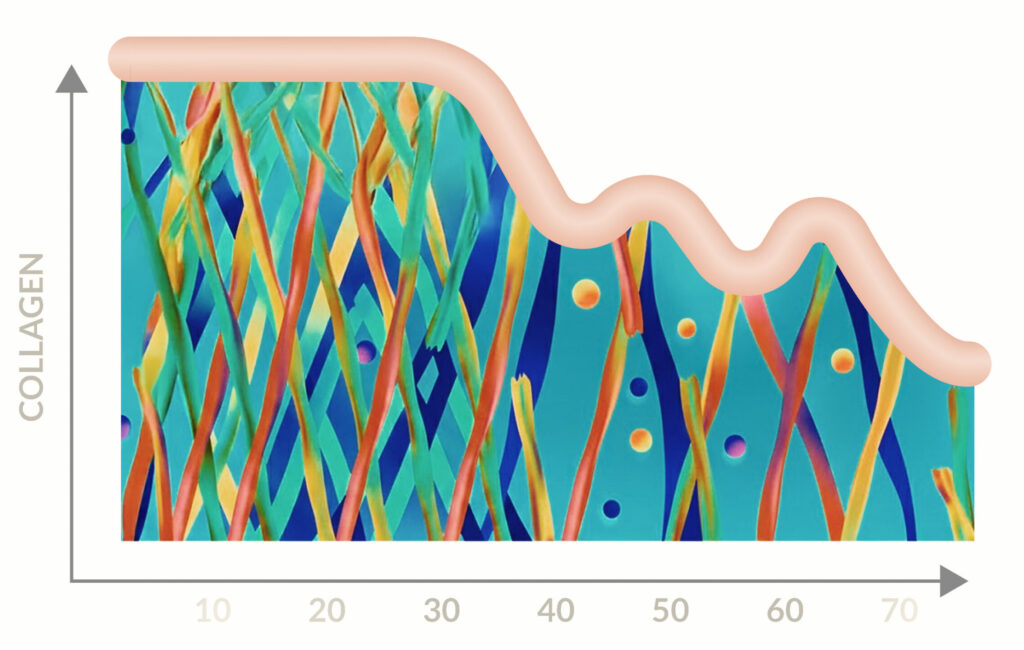
From around the age of 30, the skin loses approximately 1% of its collagen each year.
Collagen is the primary structural protein of the skin. It provides strength, elasticity and mechanical stability. As collagen levels decline, skin becomes thinner, less resilient and increasingly vulnerable to environmental damage.
While collagen loss is a natural part of aging, its speed and severity are strongly influenced by external and modifiable factors. Understanding these mechanisms is the foundation of effective prevention and long-term skin health.
Why Does Skin Lose Collagen After 30?
1. Declining fibroblast activity
Fibroblasts are the cells responsible for producing collagen and other structural components of the dermis. From the early 30s onward, their metabolic activity gradually decreases. Skin renewal slows and repair processes become less efficient.
2. Ultraviolet radiation as the main driver of collagen degeneration
Chronic UV exposure remains the most important external cause of premature collagen loss.
Ultraviolet radiation:
- activates enzymes that break down collagen fibres
- suppresses new collagen synthesis
- increases inflammation and oxidative stress
This explains why daily photoprotection is the most effective anti-aging intervention documented in dermatology.
3. Oxidative stress and lifestyle influences
Free radicals generated by pollution, psychological stress, lack of sleep, smoking and alcohol directly damage collagen structures and impair fibroblast function. Oxidative stress accelerates biological skin aging far more than many people realise.
4. Early hormonal changes
Even before menopause, subtle hormonal shifts begin in the 30s. Estrogen and growth factors play a critical role in maintaining collagen density and skin thickness. As their influence gradually declines, structural changes become more apparent.
5. Genetic predisposition – not destiny
Genetics influence baseline collagen quality and repair capacity. However, research consistently shows that the majority of visible skin aging is driven by environmental and lifestyle factors, not genetics alone.
How to Slow Collagen Loss and Support Regeneration
Aging itself cannot be stopped. However, evidence-based strategies can significantly influence how quickly collagen declines and how well the skin maintains its structure.
1. Daily photoprotection as the foundation
Consistent use of broad-spectrum SPF 50 protects collagen from UV-induced degradation and is the cornerstone of every meaningful skin health strategy.
2. Skincare ingredients with proven biological relevance
Retinoids (Retinol, Retinal, Tretinoin)
Retinoids are the most extensively studied topical agents for collagen stimulation. They activate fibroblasts, increase collagen synthesis and improve dermal thickness over time.
Vitamin C (ascorbic acid)
Vitamin C is essential for collagen formation and functions as a powerful antioxidant. It stabilizes collagen fibres and reduces oxidative damage.
Niacinamide (vitamin B3)
Improves barrier function, reduces inflammation and supports dermal integrity. Topical skincare supports collagen health, but cannot replace medical stimulation.
3. Lifestyle factors that meaningfully affect collagen
- restorative sleep
- antioxidant-rich nutrition
- regular physical activity
- stress reduction
- avoidance of smoking
- moderation of alcohol
These measures reduce oxidative stress and support long-term skin resilience.
4. Energy-based treatments for true collagen stimulation
Energy-based devices play a central role in modern collagen induction by delivering controlled physical signals to the dermis that activate fibroblasts and initiate remodelling processes. Different wavelengths target different skin depths and biological mechanisms.
Picosecond laser technology (1064 nm)
Picosecond lasers operating at 1064 nm stimulate collagen primarily through photoacoustic effects rather than thermal injury. Ultra-short pulses create mechanical stress signals in the dermis that activate fibroblasts while leaving the epidermis largely intact.
This approach is particularly suitable for:
- early collagen decline
- prevention-focused strategies in the 30s
- patients seeking stimulation without significant downtime
Non-ablative fractional laser (1550 nm)
The 1550 nm fractional wavelength delivers controlled thermal energy into the dermis while preserving the epidermis. It is well established for inducing deep dermal collagen remodeling. Clinical effects include improved skin density, firmness and long-term structural strengthening, making it a cornerstone of regenerative strategies when collagen loss becomes clinically visible.
IPL and collagen – a supportive effect
Intense Pulsed Light primarily targets pigment and vascular changes. While its collagen-stimulating effect is modest, repeated treatments may contribute indirectly to dermal health by reducing inflammation and improving overall skin quality.
CO₂ laser technology – advanced collagen remodelling in selected cases
CO₂ lasers represent the most intensive form of laser-based collagen remodeling. By creating controlled micro-ablative zones, they trigger a strong wound-healing response and deep structural regeneration. With modern pulse-controlled systems, treatment intensity can range from light resurfacing to deeper fractional protocols.
In patients in their 30s, CO₂ laser resurfacing is not a first-line preventive treatment, but may be appropriate in selected cases such as early structural damage or scarring that does not respond to non-ablative approaches.
5. Injectable treatments that truly induce collagen
Certain injectable therapies act directly on fibroblast activity and collagen synthesis.
Polylactic acid (PLA)
Induces controlled inflammatory responses that lead to gradual, sustained collagen production.
Calcium hydroxylapatite (CaHA)
Provides immediate structural support while stimulating long-term collagen formation when used in diluted protocols.
Polynucleotides
Support cellular repair mechanisms and enhance dermal quality on a regenerative level.
What Results Are Realistic in Your 30s?
A structured, prevention-oriented approach can:
- slow collagen degeneration
- stimulate new collagen formation
- improve firmness and elasticity
- refine texture
- strengthen the skin barrier
- reduce future photodamage
The 30s represent a critical window for long-term skin health.
Conclusion
Collagen loss after the age of 30 is inevitable, but its progression is highly modifiable. With consistent photoprotection, evidence-based skincare, healthy lifestyle choices and appropriately selected medical treatments, skin structure and resilience can be preserved well into later decades. Understanding the biology of aging skin is the first step. Individual assessment and medically guided strategies form the foundation for maintaining skin health, structure and resilience over time.