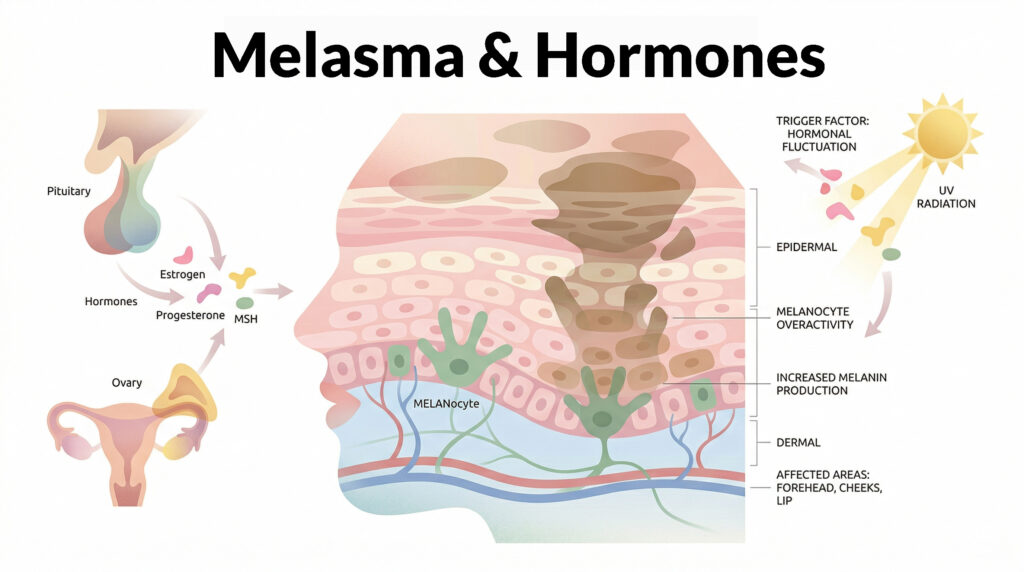
Many patients come to our clinic already knowing that melasma is “hormonal.” They have stopped the pill, invested in skincare, used sunscreen consistently — and yet the pigmentation remains.
This is often the moment when frustration begins.
Because what most women are not told is this: melasma is not just a hormonal issue. And it is not just a pigment problem. It is one of the most complex pigmentation disorders we treat in dermatology.
Melasma is more than surface pigmentation
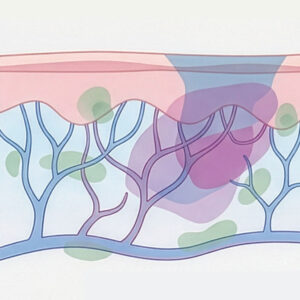
From a clinical perspective, melasma is not a uniform condition. It differs significantly in structure, depth and biological behavior. We differentiate between more superficial forms that tend to respond better to treatment and deeper forms in which pigment is deposited in the dermis and becomes significantly more difficult to influence. In many patients, these components coexist. In addition, melasma is often accompanied by a vascular and inflammatory component. This means that not only pigment cells are involved, but also blood vessels and inflammatory signaling pathways. This complexity is clinically highly relevant, because it determines both the treatment strategy and the prognosis within modern pigment therapies.
Why many treatments fail

Many patients have already tried a wide range of treatments before coming to us. They have used topical products, undergone superficial procedures or sought advice in different settings, often with the expectation that the pigmentation can simply be removed.
In reality, melasma is frequently treated too superficially. Procedures that only target the upper layers of the skin often fail to address deeper pigment deposits or the underlying biological drivers.
In clinical practice, we regularly see patients who have invested significant time and money into treatments without lasting improvement. This is not because melasma cannot be improved, but because it has not been approached at the right biological level.
Why dermatological diagnosis matters
Melasma requires precise medical evaluation. It is not enough to identify pigmentation — we need to understand its depth, its structure and the factors that maintain melanocyte activity.
A thorough dermatological assessment includes both clinical examination and a detailed medical history. Hormonal influences, sun exposure patterns, previous treatments and skin sensitivity all play a role in hormone-related skin biology.
Without this level of understanding, treatments may not only be ineffective, but can destabilize the skin further. This is one of the reasons why patients often lose confidence after multiple unsuccessful attempts.
Hormones are part of the picture — but not the whole story
Hormonal influence is a key factor in melasma, but rarely the only one. Many patients have already addressed obvious triggers such as hormonal contraception and still experience persistent pigmentation.
The reason is that the skin often remains biologically sensitized. Hormonal signaling affects melanocyte activity, vascular reactivity and inflammatory pathways, and these effects can persist even after the initial trigger has been removed.
Melasma is therefore not simply “switched off” once hormones are adjusted.
Sunlight: small exposure, big impact

Ultraviolet radiation is one of the most important external drivers of melasma. What is frequently underestimated is how little exposure is needed to reactivate pigmentation.
In sensitive skin, even short periods of daylight, incidental exposure or cloudy conditions can be sufficient to stimulate melanocytes. This is why daily, consistent photoprotection is essential — not only during holidays or in strong sunlight, but throughout the year.
The goal is not only to protect the skin, but to keep melanocyte activity as stable and inactive as possible over time.
A structured and realistic treatment approach
A meaningful melasma treatment strategy always works on several levels. It includes consistent photoprotection, a well-adapted skincare routine and targeted medical interventions when necessary.
Topical approaches can support pigment regulation and reduce inflammation, while systemic options may be considered in more resistant cases. However, no single measure is sufficient on its own. Melasma requires a combination of strategies that are carefully adapted to the individual skin condition.
Equally important is expectation management. The longer melasma has been present, the more stable and complex it becomes. The goal is therefore not immediate elimination, but gradual improvement and long-term stabilization.
Laser treatment: precision and experience are essential
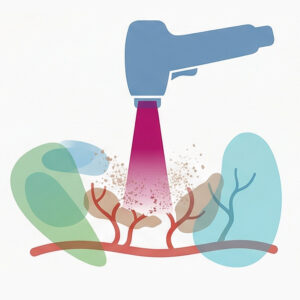
Laser therapy can be an effective part of melasma treatment — but only when used with great precision and clinical experience.
Not every laser is suitable for melasma. Inappropriate or overly aggressive treatments can worsen pigmentation by increasing inflammation or triggering melanocyte activity.
This is where specialized dermatological laser centers have a clear advantage. A broader range of technologies allows treatments to be tailored precisely within modern laser medicine.
In our clinical approach, we select devices based on the biological characteristics of the melasma. When a vascular component is present, targeted vascular treatments are integrated. For pigment modulation, modern picosecond laser technologies play a particularly important role. These systems allow controlled fragmentation of pigment with minimal thermal damage, reducing the risk of stimulating new pigmentation.
The goal is not aggressive removal, but controlled, step-by-step improvement — always embedded in a comprehensive treatment strategy.
What we see every day in practice
In daily practice at mySkin Mallorca, we very frequently see patients who have been struggling with melasma for years. Many of them are frustrated and exhausted from trying multiple treatments without lasting success.
What often changes the situation is not a single intervention, but a shift in understanding. Once melasma is approached as a chronic, biologically driven condition rather than a purely cosmetic issue, treatment becomes more structured and more effective.
A realistic and positive outlook
It is important to say this clearly: melasma cannot always be completely eliminated. In some cases, we accompany the condition over time rather than fully resolving it.
However, this does not mean that nothing can be done. With a structured, medically guided approach, we are usually able to achieve a significant aesthetic improvement and, even more importantly, greater stability of the skin.
For patients seeking a structured and medically guided melasma treatment approach, a specialized dermatological evaluation is often the most important first step.
Melasma is not about quick fixes. It is about understanding the skin, respecting its biology and working with it over time. When this approach is taken, the frustration many patients initially feel often gives way to confidence — and to visible, lasting improvement.




