Many people notice that their skin suddenly changes during stressful phases of life. The skin may look tired, breakouts appear more frequently, redness becomes more visible or dark circles deepen. These changes often seem to happen overnight.
From a dermatological perspective, however, skin rarely changes suddenly. What you see on the surface is usually the result of processes that have been building for some time. The skin is highly responsive to signals from the body. As the largest organ of the body, it reflects internal balance – or imbalance – more clearly than many people realize.
Stress hormones and the skin
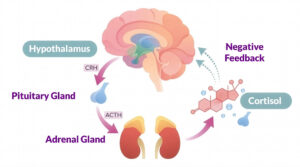
When the body experiences stress, it activates the hypothalamic–pituitary–adrenal axis. One of the main hormones released in this process is cortisol. In short bursts cortisol is helpful and necessary. But when stress becomes chronic, persistently elevated cortisol levels begin to affect many systems in the body – including the skin.
Barrier repair slows down, inflammatory pathways become more active and collagen breakdown accelerates. Over time this can lead to dullness, increased sensitivity and premature signs of skin aging. You may simply notice that your skin suddenly feels less resilient than before.
Why stress triggers breakouts and inflammatory skin conditions
One of the most visible effects of stress on the skin is inflammation. Elevated cortisol levels influence immune signaling and increase the release of inflammatory mediators. This is why many inflammatory skin conditions worsen during stressful periods.
Acne may flare during exam periods or demanding work phases. Rosacea can become more active, and inflammatory dermatitis may suddenly appear even in people whose skin was previously stable.
Perioral dermatitis is another condition we frequently observe during stressful periods. The skin around the mouth becomes red, irritated and covered with small inflammatory papules. Stress, together with barrier disruption or excessive skincare routines, can trigger or aggravate this condition. Stress does not directly cause these diseases, but it amplifies the inflammatory pathways that drive them.
Stress weakens the skin barrier
The epidermal barrier protects the body from environmental irritants, allergens and microorganisms. Under chronic stress, the skin produces fewer structural lipids such as ceramides, which are essential for maintaining barrier stability.
When the barrier becomes compromised, the skin loses moisture more easily and becomes more reactive. You may notice that the skin suddenly feels dry, sensitive or easily irritated. Products that you have used for years may suddenly start to sting or cause redness.
This situation is often mistaken for a new allergy. In reality it is frequently a sign that the skin barrier has become unstable and temporarily cannot tolerate the same level of stimulation as before.
When skincare suddenly stops working
Dermatologists often see patients who are confused because their usual skincare routine suddenly causes irritation. A cleanser, serum or cream that worked perfectly for years may suddenly trigger burning or redness.
In many cases this is not a true allergic reaction. Instead, the skin has become more reactive because the barrier is weakened by stress, inflammation or sleep deprivation. When the barrier loses stability, even well-formulated products may temporarily become too stimulating for the skin.
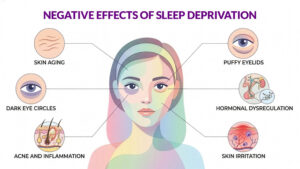
Sleep and skin regeneration
Sleep plays an important role in skin repair. During deep sleep the body activates many regenerative processes. Skin cells renew themselves, oxidative damage is repaired and collagen synthesis increases.
When sleep is shortened or repeatedly disrupted, these processes become less efficient. Over time insufficient sleep contributes to dull skin tone, reduced elasticity and more pronounced dark circles. The skin simply has less time to recover.
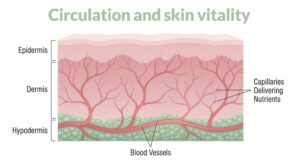
Circulation and skin vitality
Stress also affects circulation. Activation of the sympathetic nervous system causes blood vessels to constrict and redirects blood flow toward essential organs and muscles.
While this response is useful in acute danger, it reduces oxygen and nutrient delivery to the skin. Reduced microcirculation can make the skin appear pale, tired and less radiant.
Stress also changes behaviour
Stress does not only influence internal biology – it also changes everyday habits. During stressful periods people often sleep less, eat more sugar or highly processed foods, drink more alcohol and neglect regular skincare routines.
Each of these factors affects skin health individually. When they occur together, their effects accumulate, which is why stressful phases often coincide with visible skin deterioration.
Bringing stressed skin back into balance
When the skin becomes reactive during stressful periods, the first step is usually not to add more active treatments. In many cases the barrier is already irritated and overwhelmed. The goal is to calm the skin and restore stability.
This often means temporarily simplifying the skincare routine. Strong retinoids, frequent exfoliating acids or too many layered products may further irritate already stressed skin. Hydration becomes central during this phase. Ingredients such as hyaluronic acid help restore moisture levels and support skin resilience without increasing irritation.
At the same time, many people instinctively reach for very rich creams when their skin becomes irritated. In reality, excessively heavy formulations can sometimes worsen congestion or inflammation. In most cases gentle cleansing, light hydration and barrier-supporting care are the most effective approach.
When cumulative damage has already become visible, skin rejuvenation may become part of a broader dermatological treatment strategy.
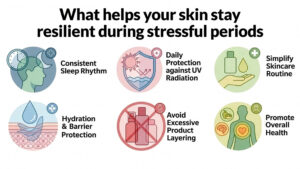
What helps your skin stay resilient during stressful periods
Stress cannot be eliminated completely, but you can support your skin’s ability to cope with it. From a dermatological perspective, a few principles make a significant difference.
- Maintain a consistent sleep rhythm whenever possible
- Protect the skin daily from ultraviolet radiation
- Simplify skincare routines when the skin becomes reactive
- Focus on hydration and barrier support rather than strong active ingredients
- Avoid excessive layering of products during inflammatory phases
- Support overall health through balanced nutrition and stress regulation
When the skin barrier stabilizes and inflammation decreases, the skin usually regains its natural balance faster than many people expect.
The skin reflects the body’s overall balance
Ultimately the skin tells a story about the body’s overall state. It reflects not only age or genetics but also sleep, nutrition, hormones and emotional well-being. When you learn to interpret these signals, skincare becomes more than cosmetic care. It becomes part of maintaining the body’s broader health and balance.
For long-term prevention, daily photoprotection and regular skin cancer prevention remain central pillars of responsible skin care.
In selected cases, supportive regenerative aesthetic treatments may complement a broader strategy when structural resilience needs additional support.